
Asthma: When breathing becomes a battle. How to help someone having an asthma attack.
Asthma is something most of us will come across at some point in our lives.
In the UK, around 1 in 9 adults live with asthma. That is millions of people managing a condition that, on a good day, is controlled and barely noticeable… and on a bad day, can become frightening very quickly.
As always, my aim is simple. Keep it practical. Keep it clear. Give you something you’ll actually remember if you ever need it. Because when someone is struggling to breathe, confidence matters.
Let’s break it down properly.
What Is Happening During an Asthma Attack?
Asthma affects the airways in the lungs. When someone has an asthma attack:
- The muscles around the airways tighten.
- The lining becomes swollen and inflamed.
- Extra mucus is produced.
All of that means the airway narrows. Air struggles to move in and out. Breathing becomes hard work.
And when breathing becomes hard work, panic often follows, which can make everything worse.
Recognising an Asthma Attack
Asthma attacks are not always dramatic or obvious. Sometimes it starts subtly.
Look for:
- Difficulty breathing or speaking. They may pause mid-sentence to catch their breath.
- Wheezing. That high-pitched whistling sound.
- A tight chest.
- Persistent coughing.
- Pale or clammy skin.
- Blue lips in more severe cases.
- Struggling to breathe, using neck and chest muscles.
- Extreme tiredness or confusion.
- Becoming unresponsive or losing consciousness in prolonged, untreated attacks.
If someone says, “I can’t breathe properly,” believe them. Don’t minimise it.
Asthma can escalate quickly.
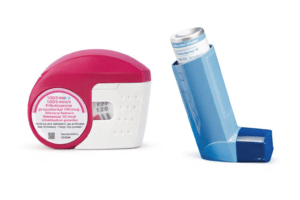
Reliever vs Preventer: Not All Inhalers Are the Same
Traditionally, most people carried:
- A blue reliever inhaler (usually salbutamol) for quick symptom relief.
- A preventer inhaler is taken daily to reduce inflammation.
But asthma management has evolved.
Let’s Talk About MART Inhalers
You may now hear about something called a MART inhaler.
MART stands for Maintenance and Reliever Therapy.
This is a combination inhaler that contains:
- A low-dose steroid (to reduce inflammation), and
- A fast-acting bronchodilator (to open the airways).
Instead of having separate blue and brown inhalers, some people now use one combination inhaler both daily and as needed during symptoms.
This is important from a first aid perspective.
If someone tells you they use a MART inhaler, that inhaler is their reliever. It might not be blue. Do not assume blue equals emergency and brown equals routine. Always ask:
“Which inhaler do you use for symptoms?”
Follow their asthma action plan if they have one.
UK guidance increasingly supports MART therapy because it can reduce severe attacks and hospital admissions when used correctly. But from a first aid point of view, the principle is still the same: help them use the inhaler they rely on for relief.
What To Do If Someone Is Having an Asthma Attack
Stay calm. Your calm helps them stay calm.
1. Sit Them Upright
Do not lie them down.
Help them sit upright, slightly leaning forward. Resting their arms on a table can help ease breathing.
2. Use Their Reliever Inhaler
This might be:
- A blue inhaler, or
- Their MART combination inhaler.
Blue Riliever inhaler – Give 1 puff of their inhaler every 30 to 60 seconds, up to 10 puffs.
MART – give one puff every 1 to 3 minutes up to six puffs.
Use a spacer if they have one. It helps the medication reach the lungs more effectively.
Encourage slow, steady breaths.
3. Call 999 or 112 If:
- There is no improvement after 10 puffs.
- They are getting worse at any point.
- You are unsure.
- This is their first attack.
- They do not have their inhaler.
If the ambulance has not arrived and symptoms continue, you can repeat up to 10 puffs every 30 to 60 seconds.
Do not just give one puff and hope for the best. Stay with them. Monitor them.
What Not To Do
- Do not take them outside into cold air. Cold air can trigger or worsen bronchospasm.
- Do not leave them alone.
- Do not assume they are “just panicking”.
- Do not delay calling for help if they are deteriorating.
If They Become Unconscious
If they collapse:
- Open the airway.
- Check breathing.
- If they are not breathing normally, start CPR and follow emergency services instructions.
Asthma can be life-threatening. Early action saves lives.
A Quick Word on Asthma Action Plans
Many people with asthma have a written asthma action plan provided by their GP or asthma nurse. It outlines:
- What inhaler to use
- How many doses
- When to seek urgent help
In workplaces, schools, care settings, and public-facing roles, knowing how to support someone with asthma is part of being prepared.
If you work in health and social care, education, or any environment with vulnerable individuals, this is not just helpful knowledge. It is essential.
Why This Matters
Asthma deaths are rare, but they do still happen. Often, there were missed warning signs or delays in treatment.
The good news? Most asthma attacks respond well to prompt inhaler use.
You do not need to be a clinician to make a difference. You just need to:
- Recognise it.
- Act early.
- Stay calm.
- Know when to call for help.
Simple. Practical. Memorable.
Because when someone is fighting for breath, you do not want to be Googling what to do.
You want to already know.
Written by Stephanie Austin – Founder & Lead Trainer, Prima Cura Training
Stephanie Austin has over 25 years’ experience in health and social care and nearly 20 years of teaching first aid. She holds the full TAQA suite of qualifications. Read more about Stephanie’s qualifications and professional background here.
Last reviewed: February 2026
Last Updated: 11th February 2026
Reviewed against: NHS guidance, Asthma UK
Disclaimer: Information shared here reflects current UK guidance at the time of writing and is for education only, not a replacement for professional training or medical advice.




